
The recent reorganisation of care for severely burned children at CHUV, covered by RTS, looks at first like a clinical story.
A rare and complex expertise being concentrated in highly specialised teams.
But this kind of news often points to something else as well.
It reminds us that as healthcare systems become more specialised, the challenge is no longer only about bringing the right experts together.
It is increasingly about a very practical question.
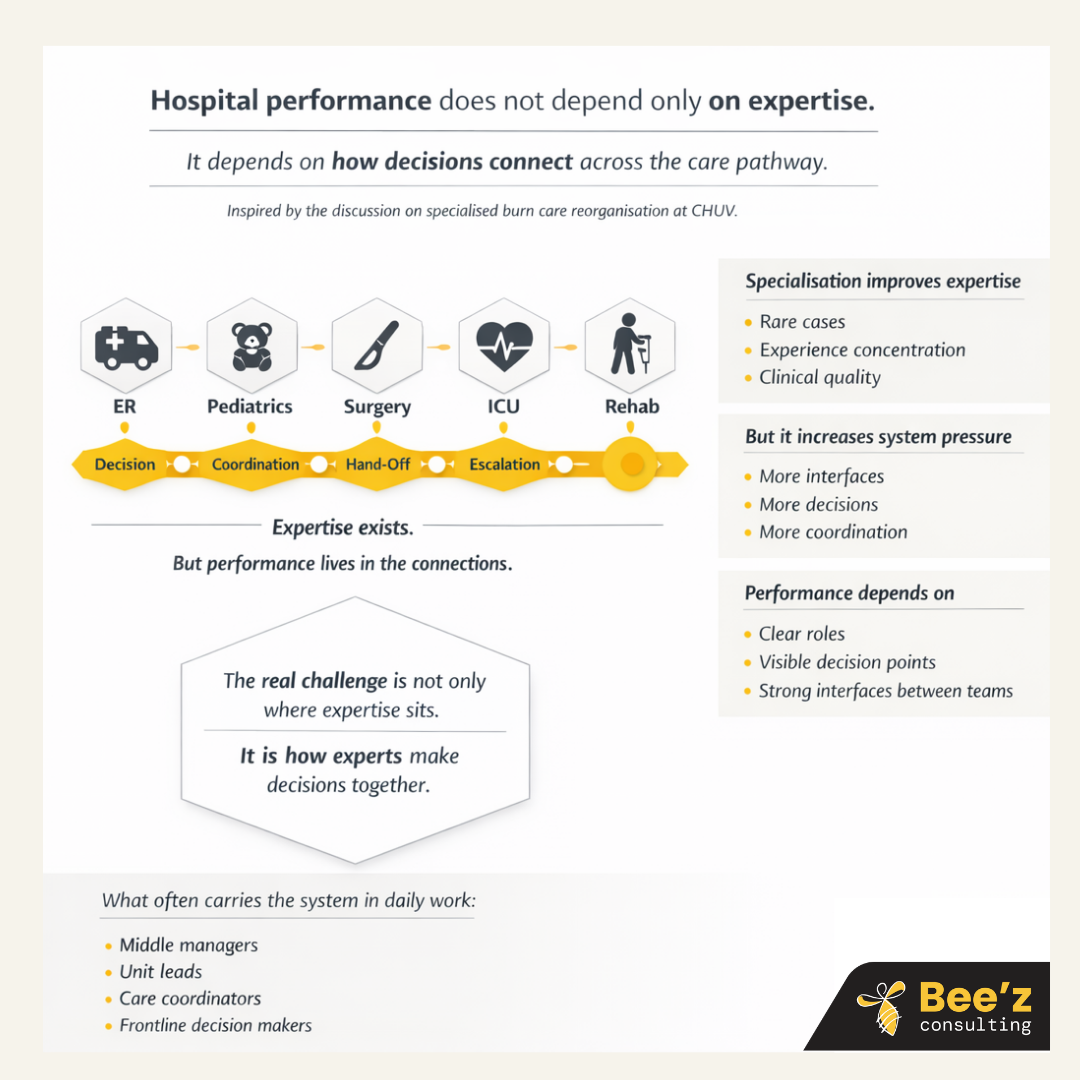
How do their decisions connect in day-to-day operations?
This is often where organisations begin to feel the pressure.
On paper, concentrating expertise makes sense.
For rare and critical cases, bringing experience together often improves clinical outcomes.
But the more expertise concentrates, the more demanding the system becomes in another way.
It starts depending on interfaces, handovers, trade-offs between teams, and decisions that need to move quickly and clearly.
And this is often where the real difference appears between an organisation that is highly expert and one that can also hold the full pathway together.
Concentrating some complex cases in highly specialised centres makes sense.
In rare and critical situations, accumulated experience often improves clinical quality.
But that logic creates another requirement.
The more expertise concentrates, the more the system depends on the quality of its links.
For example, between:
In other words, performance no longer depends only on the quality of each expertise taken separately.
It depends on how decisions move between them.
In many healthcare organisations, lack of expertise is not the main issue.
What tends to create strain more often is the way decisions move when several teams need to work together.
The same questions come up quickly:
When these points are unclear, teams compensate.
The system keeps moving.
But it moves because of people, not because of clarity.
And that is often where fatigue starts to build.
For the institution, a complex case is a sequence of specialised acts.
For patients and families, it is a pathway.
And that pathway is not shaped only by the quality of each clinical act.
It is also shaped by what connects the steps.
The questions are simple:
When governance is clear, the pathway feels more fluid.
When it is not, patients and families quickly feel the seams of the system.
We often talk about quality in terms of expertise, protocols and clinical safety.
Of course these matter.
But for patients, quality is also measured in lived continuity.
And that continuity also depends on how expertise is governed.
The other signal is just as concrete.
In highly specialised environments, professionals usually do not lack knowledge.
What they more often lack is clarity around decisions.
When these markers are clear, teams move faster and with less friction.
When they are not, the load does not disappear.
It moves downward in the system.
It lands on:
These are the people who connect worlds.
They absorb tensions.
They translate priorities into action.
This is where the issue quickly becomes a management issue.
Because a hospital can have excellent experts and still wear teams down if coordination keeps relying on improvisation.
Operational excellence is still too often reduced to tools, processes or efficiency gains.
In complex healthcare systems, it starts lower down and in a much more practical place.
It starts when critical decisions are made:
That requires at least three things.
Without that, strategy stays at the top while friction spills downward.
Organisations announce concentration of expertise.
Then, on the ground, teams are asked to hold together what the organisation has not clarified enough.
This is exactly where strategy gets lost in operations.
This is also where one of the most underestimated layers of the system sits.
Middle management.
In hospitals, they are often the people who make specialisation actually work.
Not in presentations.
In real life.
In practice:
And yet they are still too rarely equipped for this role.
They are expected to coordinate expertise, regulate tensions, support pressured teams and keep things moving.
Often without clear frames, without a shared language and without enough practice space.
In a specialised system, that is a real risk.
Because middle managers are not just one more administrative layer.
They are often the hinge of execution.
There is another angle that organisations still underestimate.
When governance is unclear, it does not only create delays.
It also creates a climate.
When roles are clear and decisions move more smoothly, teams experience something different.
In other words, the way expertise is governed also shapes the emotional culture of work.
And that culture directly influences the quality of coordination.
Teams do not make the same decisions when they feel supported as when they feel alone, exposed or under constant strain.
The CHUV story is not only about one area of paediatric burn expertise.
It reminds us of something broader.
As healthcare systems become more specialised, the central question is no longer only:
Where does expertise sit?
The real question becomes:
How do we help that expertise make good decisions together, quickly, without exhausting teams or weakening the patient pathway?
This is a governance question.
It is an execution question.
And very concretely, it is a middle management and workplace culture question.
At Bee’z, this is a pattern we often see with healthcare organisations.
A great deal gets invested in structures, expertise and tools.
Much less gets invested in the layer that connects all of this in daily work.
And yet that is often where performance holds or starts to slip.
Not only in individual competence.
In the collective ability to decide, coordinate and act under pressure.
This is why we put so much focus on:
Because a highly specialised system does not hold together through experts alone.
It holds together through the quality of the links between them.

%20(1).png)
Two years of Forbes and Statista data show the same pattern. Pharma near the top. Hospitals further down. The gap is not about mission or values. It is structural. Here is what it reveals and what to do about it.

%20(1).png)
Patient experience often breaks in the gaps between teams, not in a single interaction. Here are three practical shifts that help healthcare leaders improve handoffs, reduce escalation, and make coordination work better.


When expertise concentrates in hospitals, the real challenge becomes coordination. Governance, middle management, and emotional culture shape outcomes for both teams and patients.
